Clinical
The OCULUS Myopia Master in Action - Q&A with Max Aricochi
Sponsored by
In this article:
We explore the OCULUS Myopia Master with practical questions of how optometrist Max Aricochi uses it in his clinic in Austria.
Our new Q&A format is designed to explore a particular clinical topic, intervention, product or research paper with an expert. Here, we explore the OCULUS Myopia Master with practical questions of how optometrist Max Aricochi uses it in his clinic in Austria. We also provide you some additional tips to help you put Max's recommendations to use in your own practice.
How do you describe axial length measurement to parents and patients?
As most parents are not familiar with axial length, Max suggests using a child's height as an analogy - that just as a child grows taller, their eyes also grow longer, following a trajectory that can be plotted as a growth curve. Parents are quite familiar with percentile growth curves for height and weight so translating that to axial length elongation is straight forward. A study has also showed that there is correlation between body growth and axial elongation, so this analogy is a reasonable comparison.1
Helping parents understand the importance of measuring axial length is also very useful for determining management outcomes. This provides an objective measure which can form a baseline, and to consider this alongside progression noted in refractive error.
Do you have any tips for taking swift and accurate measures for kids?
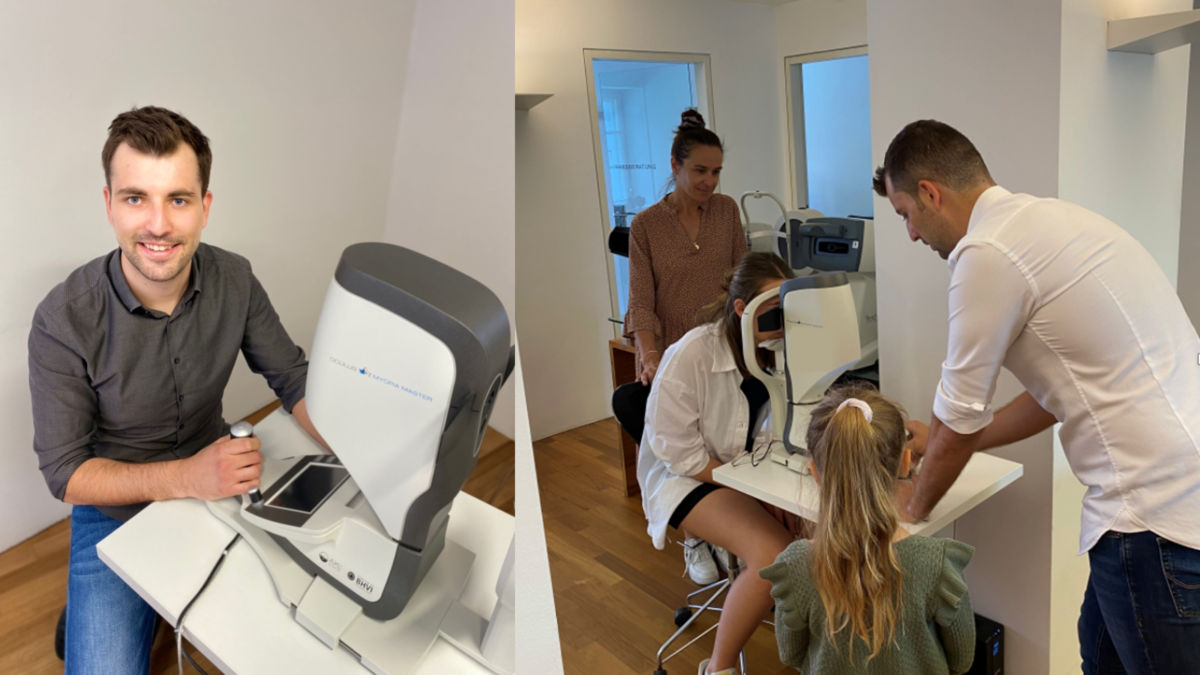
As shown in the image above, the child can be stabilised by placing the hands on the side pieces of the machine and placing the chin flush on the chin rest. The parent may support their child's head so it is against the forehead rest. The child can then be instructed to look directly at the target so the measurement can be taken.
How do you explain the results of the OCULUS Myopia Master with parents and patients?
The image above shows one of the output screens of the Myopia Master used in Max's practice (in the German language), where the axial length measurement is transferred to a growth chart. The solid bold black line is the mean axial length (i.e. 50th percentile) for a child of that sex and ethnicity, whilst the upper and lower lines represent the 95th and 5th percentile respectively. The parents then are able to compare their child's axial length with Myopia Master database, which consists of 14,127 Asian eyes and 7,204 European eyes. This growth chart also predicts the axial length in adulthood depending on the child's percentile result and their growth trajectory.
For this example provided by Max, both right (R) and left (L) eyes of this patient, who has a current age of 9 years, have an axial length on the highest percentile. The dotted purple and blue lines track along this highest percentile to a prediction of very high myopia by adulthood, with the bracket indicating the potential range of outcomes.
Have you found parents respond more to certain aspects of Myopia Master reports?
Parents have been quite impressed by the explanation of the statistic data [the growth chart], as is interesting for both parents with statistical background as for parents without - even for them it is well explained. The function that really stands out in the Myopia Master is the GRAS Module. It allows me to provide more thorough myopia management communication, because it differentiates refractive from axial myopias. The optical components of the child's eye are split up into their optical components, so one can exactly see where the myopia is coming from.
The Myopia Report contains a variety of data which is useful for practitioners as well as parents. The image below shows an output Myopia Report from Max's practice (in the German language) which shows the GRAS (Gullstrand Refractive Analysis System) Module.
The purpose of the GRAS Module is to show how the individual optical components of the eye contribute to the overall refractive outcome. The individual components of axial length, corneal curvature and crystalline lens power are included, and compared to an age-referenced normal eye. In this example provided by Max, both eyes have a -3.00D refraction but the axial length is shown to be more typical for a more myopic eye. This higher-than-expected axial length indicates an increased risk of myopia-associated eye diseases,2 so helps to direct more proactive clinical care.
Do you measure axial length in adults as well as children?
It is useful to obtain axial length of both children and adults. For adults, even if their axial length is no longer growing, having this measurement can help to direct best-practice clinical care. Cases where this could be particularly important are for adults with flat corneas and lower levels of myopia, who could still have long axial length. Having this clinical data can help to establish their risk profile for myopia complications, and inform ongoing management.
How do the OCULUS Myopia Master results guide your treatment decisions?
As mentioned by Max, axial length describes the risk for 'real' myopic problems as it has a closer correlation to the lifelong risk of eye disease and visual impairment and myopia than does the refractive value of myopia.2
The International Myopia Institute Clinical Management Guidelines recommend ongoing review of children with myopia every six months. Measuring axial length every six months will help monitor the progression. This can then help to gauge success in myopia management strategies while also supporting clinical communication to patients and parents.
Meet the Authors:
About Max Aricochi
Max Aricochi is an Optometrist practicing in Innsbruck, Austria, with a keen interest and busy clinic in childhood myopia management. Max completed the M.Sc. Vision Science and Business (Optometry) at Aalen University, Germany, in cooperation with the two partner Universities, New England College of Optometry (Boston, USA) and Pacific University (Oregon, USA). He has been actively involved in myopia management since 2015. For his recent Master's Thesis, Max created a manual for myopia management in the German language, which covers this extensive and very current topic across almost 200 pages.
This content is brought to you thanks to an educational grant from
References
- Kearney S, Strang NC, Cagnolati B, Gray LS. Change in body height, axial length and refractive status over a four-year period in caucasian children and young adults. J Optom. 2020 Apr-Jun;13(2):128-136. (link)
- Tideman JW, Snabel MC, Tedja MS, van Rijn GA, Wong KT, Kuijpers RW, Vingerling JR, Hofman A, Buitendijk GH, Keunen JE, Boon CJ, Geerards AJ, Luyten GP, Verhoeven VJ, Klaver CC. Association of Axial Length With Risk of Uncorrectable Visual Impairment for Europeans With Myopia. JAMA Ophthalmol. 2016;134(12):1355-1363. (link) [Link to Myopia Profile Science Review]
Enormous thanks to our visionary sponsors
Myopia Profile’s growth into a world leading platform has been made possible through the support of our visionary sponsors, who share our mission to improve children’s vision care worldwide. Click on their logos to learn about how these companies are innovating and developing resources with us to support you in managing your patients with myopia.











