Clinical
Retinal detachment in children
In this article:
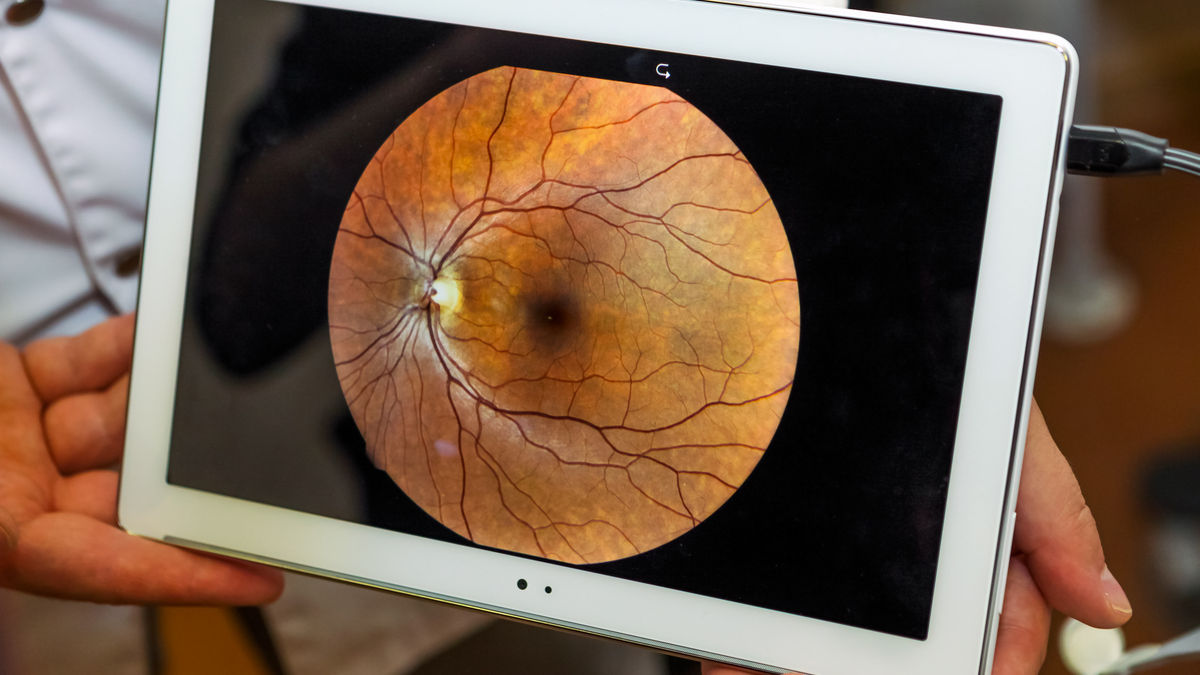
High myopes have 5-6 times higher risk of developing retinal detachments compared to low myopes.1 They also happen in adult myopes, right? Wrong! Retinal detachments can happen at any age, including in children. KG shared detail of a patient who was diagnosed with a retinal detachment at 12 years of age. Here is the case.
Retinal detachment in children
Paediatric retinal detachment (PRD) is rare and challenging. It accounts for 3%-7% of all retinal detachment cases.2 The causative factors 2 include:
- Trauma
- An associated condition (Morbus Stickler, Marfan Syndrome, Coat disease etc)
- High myopia
- Retinopathy of prematurity (ROP)
- Previous intraocular surgery
- Idiopathic
Early diagnosis can be difficult as children may not necessarily recognize or appreciate the symptoms such as a sudden increase in floaters, flashes of light, or changes in their field of vision. As a result, they may not raise the alarm that something in their vision has changed. The average age of onset of PRD is usually between 9-12 years old.3 The most common types of PRDs include: 4
- Tractional retinal detachments (29%, causes include retinopathy of prematurity, persistent fetal vasculature or familial exudative vitreoretinopathy)
- Traumatic retinal detachments (26%)
- Rhegmatogenous retinal detachments (22%, causes include myopia, X-linked retinoschisis or Stickler's syndrome)
The prognosis varies with different type of PRDs. Rhegmatogenous retinal detachments have better visual outcome whereas tractional retinal detachments have poorer visual outcome.4 In addition, late diagnosis and macular involvement also affect the outcome.
Considering the best management path
This particular child has an axial length of 26.6mm and 26.3mm in his right and left eyes respectively. As KG mentions in the original post, eyes with an axial length exceeding 26mm have an 82% frequency of retinal changes attributed to myopia, and at least a 25% cumulative risk of vision impairment across their lifetime.5,6
Attempting to control myopia as much as possible is important to reduce the continued axial growth of the patient's eyes - the mechanical impact of stretching is likely responsible for the stronger link between axial length and ocular health risk in myopia than between myopic refractive error and risk.6
Does this patient need additional myopia control intervention? The case indicates that partial correction orthokeratology has provided effective myopia control over the past 2.5 years. One commenter mentions adding 0.01% atropine, which has shown an additive effect for myopia control with orthokeratology, although this may be more in children with lower (less than 3D) than moderate myopia.7
Does this patient need additional ocular health monitoring? The answer to this is of course yes - annual retinal health examinations through dilated pupils are recommended for high myopes by the International Myopia Institute.8
Since this patient is now being co-managed between an optometrist and ophthalmologist, ongoing communication between eye care practitioners is crucial to ensure the best vision and eye health outcomes for the patient. Highly myopic patients, young or old, should be advised of the symptoms of retinal tears and detachments so that expedient clinical review is possible.
Take home messages:
- Paediatric retinal detachment may be challenging to diagnose as the symptoms are painless and children may not identify these symptoms as abnormal.
- It is important to be vigilant and perform thorough ocular health checks on all high myopes regardless of age. Retinal health examination through dilated pupils is recommended annually for high myopes, young and old.
Meet the Authors:
About Connie Gan
Connie is a clinical optometrist from Kedah, Malaysia, who provides comprehensive vision care for children and runs the myopia management service in her clinical practice.
Read Connie's work in many of the case studies published on MyopiaProfile.com. Connie also manages our Myopia Profile and My Kids Vision Instagram and My Kids Vision Facebook platforms.
About Kimberley Ngu
Kimberley is a clinical optometrist from Perth, Australia, with experience in patient education programs, having practiced in both Australia and Singapore.
Read Kimberley's work in many of the case studies published on MyopiaProfile.com. Kimberley also manages our Myopia Profile and My Kids Vision Instagram and My Kids Vision Facebook platforms.
References
- Williams K, Hammond C. High myopia and its risks. Community eye health. 2019;32(105):5. (link)
- Meier P. Retinal detachment in children: differential diagnosis and current therapy. Klinische Monatsblatter fur Augenheilkunde. 2008 Sep;225(9):779. (link)
- Nuzzi R, Lavia C, Spinetta R. Paediatric retinal detachment: a review. Int J Ophthalmol. 2017;10(10):1592. (link)
- Read SP, Aziz HA, Kuriyan A, Kothari N, Davis JL, Smiddy WE, Flynn Jr HW, Murray TG, Berrocal A. Retinal detachment surgery in a pediatric population: visual and anatomic outcomes. Retina 2018 Jul;38(7):1393. (link)
- Varma R, Meuer SM, Klein R, Wu S. Prevalence and characteristics of myopic retinopathy in an adult Chinese American population: The Chinese American Eye Study. Invest Ophthalmol Vis Sci. 2014 Apr 30;55(13):3615. (link)
- Tideman JW, Snabel MC, Tedja MS, Van Rijn GA, Wong KT, Kuijpers RW, Vingerling JR, Hofman A, Buitendijk GH, Keunen JE, Boon CJ. Association of axial length with risk of uncorrectable visual impairment for Europeans with myopia. JAMA Ophthalmol. 2016 Dec 1;134(12):1355-63. (link)
- Kinoshita N, Konno Y, Hamada N, Kanda Y, Shimmura-Tomita M, Kaburaki T, Kakehashi A. Efficacy of combined orthokeratology and 0.01% atropine solution for slowing axial elongation in children with myopia: a 2-year randomised trial. Sci Rep. 2020 Jul 29;10(1):12750. (link)
- Gifford KL, Richdale K, Kang P, Aller TA, Lam CS, Liu YM, Michaud L, Mulder J, Orr JB, Rose KA, Saunders KJ, Seidel D, Tideman JWL, Sankaridurg P. IMI - Clinical Management Guidelines Report. Invest Ophthalmol Vis Sci. 2019 Feb 28;60(3):M184-M203. (link)
Enormous thanks to our visionary sponsors
Myopia Profile’s growth into a world leading platform has been made possible through the support of our visionary sponsors, who share our mission to improve children’s vision care worldwide. Click on their logos to learn about how these companies are innovating and developing resources with us to support you in managing your patients with myopia.











