Clinical
Spectacles to contacts - what happens to BV?
In this article:
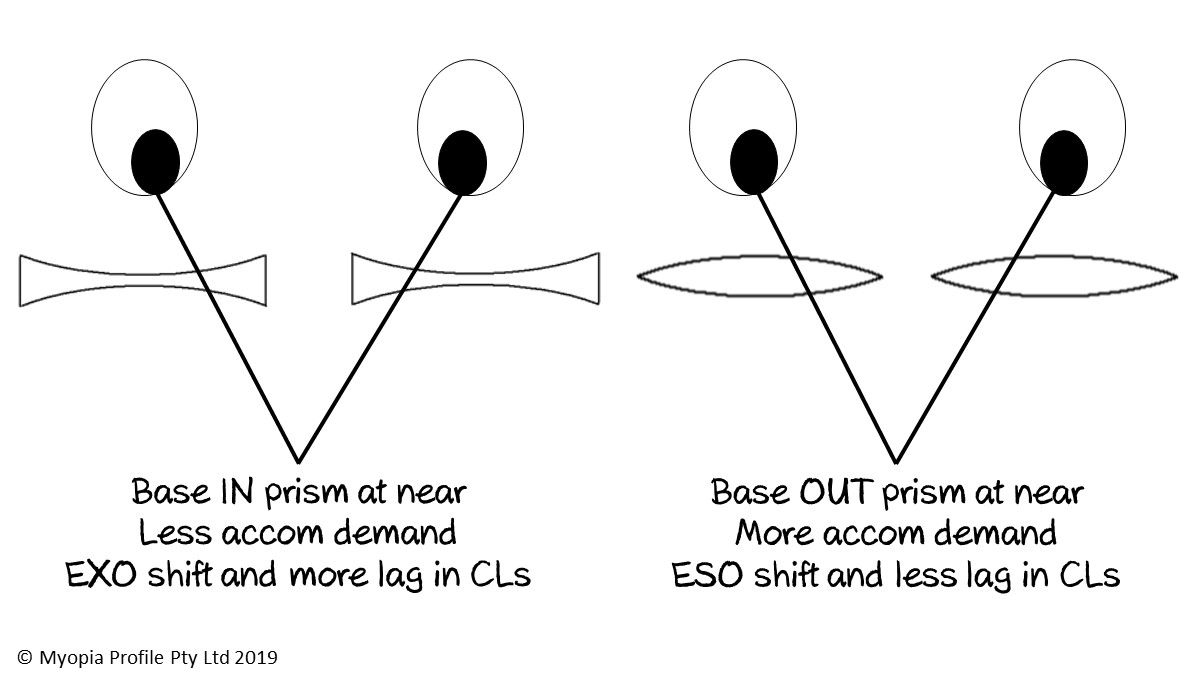
Changing a myope from spectacle to contact lens wear can alter their binocular vision (BV) function. The myope reading through their spectacles experiences base-in prism at near, as demonstrated in the image above, which moves the image further away and decreases vergence demand. Looking away from the optical centre of the lens (while keeping the vertex distance constant) also reduces the power, effectively reducing the accommodative demand. When this myope changes to a single vision distance (SVD) contact lens, he or she must increase their accommodation, which is why the early presbyopic, moderate to high myope always needs an add in their contact lenses before they do in their spectacles - and the high myopes can sometimes survive presbyopia without ever needing progressive spectacles.
Hence myopes of any age must increase accommodation demand in a SVD contact lens correction; they will show an exophoric shift in contact lenses as they lose the base-in spectacle correction and have to converge more by themselves.1 This can be beneficial to moderate-to-high myopes with esophoria in spectacles, where the spectacle-to-contact lens effect will be greater, and given that esophoria at near has been associated with a higher rate of myopia progression in SVD spectacles.2 These theoretical calculations have been confirmed experimentally in young adult contact lens wearers, with the differential between spectacle and contact lens binocular vision function at near generally increasing with increasing contact lens power, although it varies between individuals.1
Sienna's story - the myope
Sienna first presented at age 16, with progressing myopia and complaints of unstable distance vision in her glasses. Cover test quickly revealed the problem - a significant divergence insufficiency esophoria, breaking into an intermittent esotropia, worse at distance than at near. She was keen on getting rid of her -4.50 glasses and into full time contact lens wear. In Sienna's case contact lens wear served a double benefit through meeting her needs for refractive correction as well as partially remediating her binocular vision problem. Additional management was required in the form of vision training and base-out relieving prism over-specs for the classroom until her eye control improved. Four years later, Sienna is now studying at university and still wears her relieving prism spectacles sometimes in very large lecture theatres to give her binocularity the support required, but otherwise is thrilled being a full time orthokeratology (OK) lens wearer with no myopia progression noted in that time.
Simply changing from specs to contact lenses, even if they were SVD CL's, would have done something to reduce Sienna's esophoria. OrthoK (OK) and multifocal soft CLs (MFSCLs), which of course we're much more likely to fit to a young myope, have been shown to additionally improve esophoria and accommodative lag in comparison to SVD CLs, although not as may be predicted by the labelled 'add' power of a MFCL,3-6 or central refractive power of the OK treatment.7-9 MFSCLs may even increase accommodative lag - some research has shown children and young adults may relax their accommodation and use the 'add' of the lens at near.5,6 So while a myopia controlling CL may have an additional effect on BV than a SVD CL, it may not be a clinically significant or predictable additional effect. Read about Oliver's story, another esophoric myope, in The esophoric myope and contact lenses.
Brooke's story - the hyperope
Yes, I know this website is called 'Myopia Profile', but a case for hyperopia helps to paint the picture on both sides of emmetropia! Brooke has worn spectacles full time since she was 6, with her prescription at age 15 being R +4.75 and L +5.00. She's been lucky enough not to suffer amblyopia or esotropia as many of her similarly hyperopic counterparts - with her distance refraction she exhibits a moderate exophoria at near. She was first fit with daily disposable lenses for tennis when she was 12, worn twice a week. An increase in schoolwork demand saw her convergent (base-out) fusional reserves reduce, which are required to keep an exophoria in check, and as her confidence increased she was keen for more full time wear of her contact lenses. In comparison to single vision spectacle lens wear, Brooke's exophoria decreased and her convergence improved in contact lens correction, leading to a both a better aesthetic and binocular vision result in contact lens correction.
When a hyperope wearing spectacles looks at a near target, their convergence away from the optical centre of the lenses creates base-out prism in each eye, with the base being the thicker part of the lens at the centre (see picture above). This base-out prism moves the image inwards and so decreases the divergence demand. When this hyperope then switches to contact lens wear they have to diverge more by themselves, which if they are capable, will result in an esophoric shift.10 In Brooke's case, fitting her with contact lenses improved her satisfaction with her correction as well as her binocular vision function - symptomatic convergence insufficiency has been associated with reading behaviours of avoidance in children.11
BV matters for CL success
In summary, when switching from specs to contact lenses, the myope will show an exophoric shift and the hyperope an esophoric shift. There may also be effects on accommodation - more accommodative demand and hence more lag for the myope; less accommodative demand and hence less lag for the hyperope. Whether you're fitting children or adults with contact lenses, your new contact lens wearing patient can show alterations in their BV and this is more likely in higher refractions. Research has shown a correlation between contact lens discomfort and binocular vision disorders, with the authors stating that a similar set of symptoms could lead a clinician to confuse a BV disorder for a dry eye diagnosis.12 If you want your CL wearer to be successful and comfortable, it's worth evaluating their BV.
Read more about accommodation, binocular vision and myopia:
Watch these Myopia Profile YouTube videos on binocular vision techniques:
Want to learn more about binocular vision?
Check out my online course Binocular Vision Fundamentals, which starts with my two-system approach to BV assessment and diagnosis. Stepping through understanding of the accommodation and vergence systems, the course then covers clinical tests, diagnostic criteria, prescribing and management. Once this foundation is set, it moves onto clinical communication and the importance of BV in myopia management. Always with a laser sharp focus on the clinical applications.
Included are video examples of assessment techniques and chairside infographic summary downloads to reference in practice.
You can enroll on the first two modules for free, with the full course priced at US$140 if you decide to continue. Reduced course fees by 30% and 50% are available by application for practitioners residing in lower income countries - check out the course page for more information.
Meet the Authors:
About Kate Gifford
Dr Kate Gifford is an internationally renowned clinician-scientist optometrist and peer educator, and a Visiting Research Fellow at Queensland University of Technology, Brisbane, Australia. She holds a PhD in contact lens optics in myopia, four professional fellowships, over 100 peer reviewed and professional publications, and has presented more than 200 conference lectures. Kate is the Chair of the Clinical Management Guidelines Committee of the International Myopia Institute. In 2016 Kate co-founded Myopia Profile with Dr Paul Gifford; the world-leading educational platform on childhood myopia management. After 13 years of clinical practice ownership, Kate now works full time on Myopia Profile.
References
- Hunt OA, Wolffsohn JS, Garcia-Resua C. Ocular motor triad with single vision contact lenses compared to spectacle lenses. Cont Lens Anterior Eye. 2006;29:239-245. (link)
- Yang Z, Lan W, Ge J, Liu W, Chen X, Chen L, Yu M. The effectiveness of progressive addition lenses on the progression of myopia in Chinese children. Ophthal Physiol Opt. 2009;29:41-48. (link)
- Tarrant J, Severson H, Wildsoet CF. Accommodation in emmetropic and myopic young adults wearing bifocal soft contact lenses. Ophthalmic Physiol Opt. 2008;28:62-72. (link)
- Aller TA, Liu M, Wildsoet CF. Myopia Control with Bifocal Contact Lenses: A Randomized Clinical Trial. Optom Vis Sci. 2016;93:344-352. (link)
- Gong CR, Troilo D, Richdale K. Accommodation and Phoria in Children Wearing Multifocal Contact Lenses. Optometry and Vision Science. 2017;94:353-360. (link)
- Kang P, Wildsoet CF. Acute and short-term changes in visual function with multifocal soft contact lens wear in young adults. Cont Lens Anterior Eye. 2016;39:133-140. (link)
- Gifford KL GP, Hendicott PL, Schmid KL. Near binocular visual function in young adult orthokeratology versus soft contact lens wearers. Cont Lens Anterior Eye. 2017;40:184-189. (link)
- Gifford KL GP, Hendicott PL, Schmid KL. Binocular visual function in orthokeratology contact lens wear for myopia. Invest Ophthalmol Vis Sci. 2017;58:ARVO E-Abstract 2683878. (link)
- Tarrant J, Liu Y, Wildsoet CF. Orthokeratology Can Decrease the Accommodative Lag in Myopes. Invest Ophthalmol Vis Sci. 2009;50:4294. (link)
- Bennett AG, Rabbetts RB: Clinical Visual Optics. 2 ed. London; Boston, Butterworths; 1989. (link)
- Borsting E, Mitchell GL, Kulp MT, Scheiman M, Amster DM, Cotter S, Coulter RA, Fecho G, Gallaway MF, Granet D, Hertle R, Rodena J, Yamada T. Improvement in academic behaviors after successful treatment of convergence insufficiency. Optometry and vision science : official publication of the American Academy of Optometry. 2012;89:12-18. (link)
- Rueff EM, King-Smith PE, Bailey MD. Can Binocular Vision Disorders Contribute to Contact Lens Discomfort? Optom Vis Sci. 2015;92:e214-221. (link)
Enormous thanks to our visionary sponsors
Myopia Profile’s growth into a world leading platform has been made possible through the support of our visionary sponsors, who share our mission to improve children’s vision care worldwide. Click on their logos to learn about how these companies are innovating and developing resources with us to support you in managing your patients with myopia.











